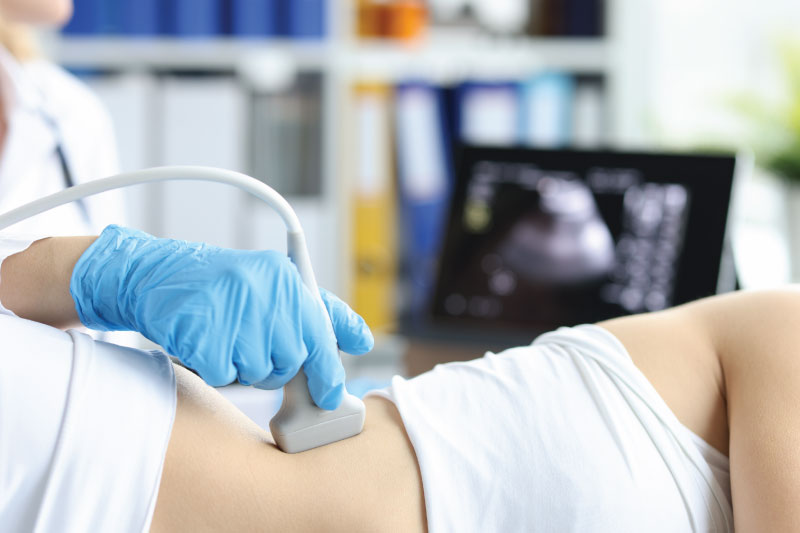
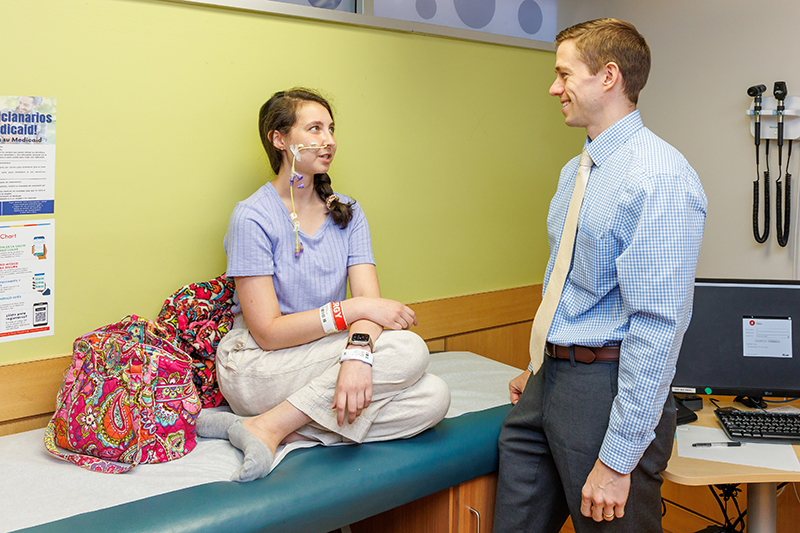
Children’s is using telehealth to answer parents’ questions about bathroom habits. (Stock photo)
For families of children with bladder and bowel dysfunction, the journey to care at Children’s of Alabama can involve a long drive, a crowded waiting room, and the worry that the problem was serious—only to be told that what their child needs most is better bathroom habits.
“We have a really wide catchment area,” said Children’s chief of pediatric urology Stacy Tanaka, M.D. “Sometimes we were seeing families coming in from the coast. They had driven three-and-a-half, four hours.” By the time they arrived, parked and waited, an entire day was lost and the advice they received was, well, less than earth-shattering.
“They get here, and you tell them, ‘Hey, you just need to urinate and poop a little bit better,’” she said. “It doesn’t go over that well sometimes.” In fact, it could have been handled by a phone call.
Today, that’s essentially how they handle it. Tanaka and nurse practitioner Kelsey Boswell Moore, CRNP, see more than 20 patients each week via telehealth.
The program launched in early 2025, partly out of necessity. “We were transitioning and were a bit understaffed,” Tanaka said. “We started it just as a ‘let’s try to get as many patients seen as possible.’”
What began as a staffing solution quickly became a new model of care.
One reason it works so well is that most children with bladder and bowel dysfunction improve just from counseling and conservative management on better bladder habits and better bowel habits. They don’t even require prescription medication. If any red flags pop up, such as a child who had back surgery or is having urinary tract infections with fever, the team brings them in for a face-to-face consultation. “Those are signals we need to see you sooner,” Tanaka said.
For most families, all it takes is talking and instructions.
“A lot of times they’ve never really paid attention to how often they’re going to the bathroom,” said Moore, who conducts most of the telehealth visits. “They’ll say they have urgency, or that they can’t hold it, but then you realize they’re waiting until the last minute every time.”
Telehealth makes it easier to explore those details.
“They’re sitting in their living room,” Tanaka said. “It’s a more relaxed environment. All the other distractions really go away. In that relaxed environment, it’s easier to talk about how often they’re going, when they’re going and what’s really happening,” she said.
“Sometimes they say they’ve done everything,” she said. “But the child is still drinking fluids late at night or didn’t actually go to the bathroom before bed.”
And for those who do need to be seen in person, the telehealth visit allows Moore and Tanaka to prepare for the appointment by ordering any necessary tests, which increases efficiency.
If families still want to be seen in the office or have the child undergo imaging, “We can absolutely do that,” Tanaka said. “We can rule out the scary things, and then it becomes easier to continue with telehealth knowing everything looks okay.”
“This only works if the patient and parent are engaged,” she added. “If they don’t feel right about the plan, it’s not going to work.”
And it does work. For instance, consider the 8-year-old boy with enuresis. The problem became obvious after a brief telehealth visit.
“When he woke up in the morning, he didn’t go to the restroom,” Tanaka said. “He would eat breakfast, get dressed, and the first time he went was at school.” The child had trained himself to ignore bladder signals.
The solution? A schedule. Go first thing in the morning and use the restroom at planned times during the day. Also, alert the teacher. Four weeks later, the problem was resolved.
“That family never had to step foot in the hospital,” Tanaka said.
Which, of course, is the goal.