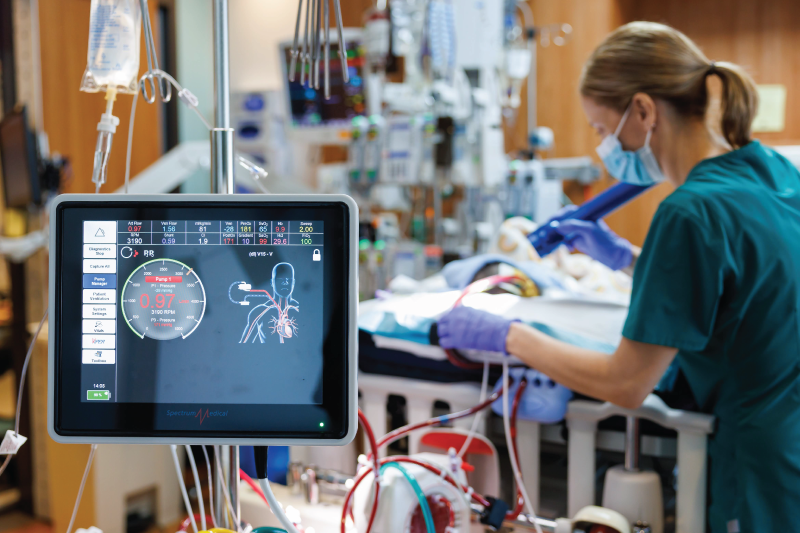
A new study is shaking up the standard practice of using heparin for anticoagulation in ECMO patients.
Anticoagulation therapy during extracorporeal membrane oxygenation (ECMO) has long relied on heparin, but a groundbreaking multicenter study co-authored by Jonathan Byrnes, M.D., medical director of cardiac ECMO at Children’s of Alabama, shows the benefits of replacing heparin with bivalirudin.
Bivalirudin isn’t a new drug, but its rise in use in pediatric ECMO stems from successes in pediatric ventricular assist devices (VADs). With earlier stroke rates as high as 25–30% on VADs using heparin, the transition to bivalirudin brought about a remarkable reduction, dropping the stroke rate to 5–8%. This significant improvement in neurological outcomes sparked interest in applying bivalirudin more extensively in ECMO settings.
The study, spearheaded by Mohammed Hamzah, M.D., of Cleveland Clinic Children’s Hospital, diverged from past practices of individual center decision-making. Instead, six medical centers collaborated, aiming to analyze outcomes through a case-matched lens, minimizing variability across patients requiring ECMO. The study’s cooperative nature across multiple centers necessitated remarkable coordination.
One of the study’s key findings, according to Byrnes, is that patients on bivalirudin exhibited lower mortality rates than those on heparin. Intriguingly, despite higher PTT levels in bivalirudin patients, they experienced less bleeding and fewer thrombotic incidents in the ECMO circuit. This hints at bivalirudin’s inherent benefits, possibly enhancing biocompatibility. “It seems that there’s something intrinsic to bivalirudin that allowed for better biocompatibility of the patient’s blood to the ECMO circuit,” Byrnes said.
The impact of this study extends far beyond the academic realm. At Children’s of Alabama, the findings suggest potential benefits such as reduced bleeding, fewer transfusions and lower mortality rates for ECMO-supported patients. However, as Byrnes noted, the retrospective nature of the study necessitates a randomized controlled trial to solidify these outcomes and effectively influence the standard of care.
Plans for a prospective trial are underway, aiming for a randomized approach coordinated through the Extracorporeal Life Support Organization (ELSO). This prospective study could validate the retrospective findings, potentially reshaping protocols for anticoagulation during ECMO.
Despite the excitement surrounding the study’s outcomes, Byrnes emphasized the need for caution. While retrospective data suggests bivalirudin’s superiority, a randomized trial is crucial to establish this definitively. Prospective data will unveil any center-specific confounders that might have influenced the study’s retrospective findings.
Byrnes underscored the significance of these findings and the hope for future randomized controlled trials. The study’s retrospective nature lays a robust foundation, but prospective data will offer irrefutable evidence to guide clinical practice, leading to a potential paradigm shift in anticoagulation therapy that may result in improved patient care and outcomes.
