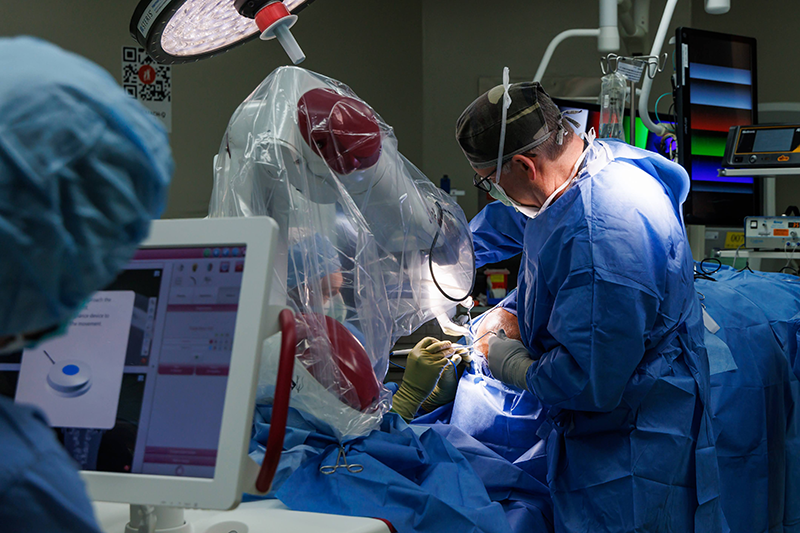
Curtis Rozzelle, M.D., performing a deep brain stimulation procedure for epilepsy.
In January 2024, a University of Alabama at Birmingham (UAB) pediatric neurosurgeon performed the first deep brain stimulation (DBS) procedure for epilepsy at Children’s of Alabama, offering a new treatment option for pediatric patients who experience drug-resistant seizures.
During the procedure, Curtis J. Rozzelle, M.D., a professor in the UAB Department of Neurosurgery, also implanted the first NeuroPace responsive neurostimulation (RNS) epilepsy treatment device at Children’s.
The NeuroPace RNS ® System, which consists of a small generator attached by leads to electrodes, was designed to communicate with a computer to record brain activity, recognize seizure-related patterns and deliver stimulation to suppress seizures. The device, which is curved for better placement within the skull, monitors brainwaves constantly and can be customized on a patient-by-patient basis.
“Much like a cardiac pacemaker that senses and responds to abnormal heart rhythms, this combination of technologies will detect brain activity that precedes seizures, then stimulate pathways deep in the brain to either prevent seizures from starting or stop seizure activity in its tracks,” Rozzelle said.
When performing a DBS procedure, a neurosurgeon inserts electrodes connected to a neurostimulator into the brain to disrupt epileptic electrical activity before it can cause a seizure. Similar to the RNS System, the DBS neuromodulation device can be programmed after placement in an outpatient clinic by an epilepsy specialist, like UAB Department of Pediatrics Division of Neurology professor Monisha Goyal, M.D.
In this case, Rozzelle placed the RNS® System electrodes in the thalamus, resulting in a twofold RNS and DBS procedure.
Neurostimulators have long been used to treat various neurological disorders when traditional treatment options fail. DBS was originally developed in 1997 to treat Parkinson’s disease and has since expanded as a treatment option for epilepsy, dystonia and more. RNS gained initial FDA approval in 2013 and has proved to be effective in many patients. Presently, RNS is FDA-approved only for adults, but is successfully being used off label in the pediatric population.
Though DBS and RNS are not viable options for all patients, they show tremendous potential in treating children with epilepsy who need more innovative treatment options. “With this first RNS implantation [at Children’s of Alabama], we have expanded the armamentarium of therapies available to individuals with poorly controlled epilepsy,” Goyal said. “Unfortunately, neuromodulation with RNS is only [FDA-approved] for individuals who are at least 18 years old. The pediatric epilepsy team at Children’s of Alabama hopes that this therapy will be available to more children of Alabama soon.”



