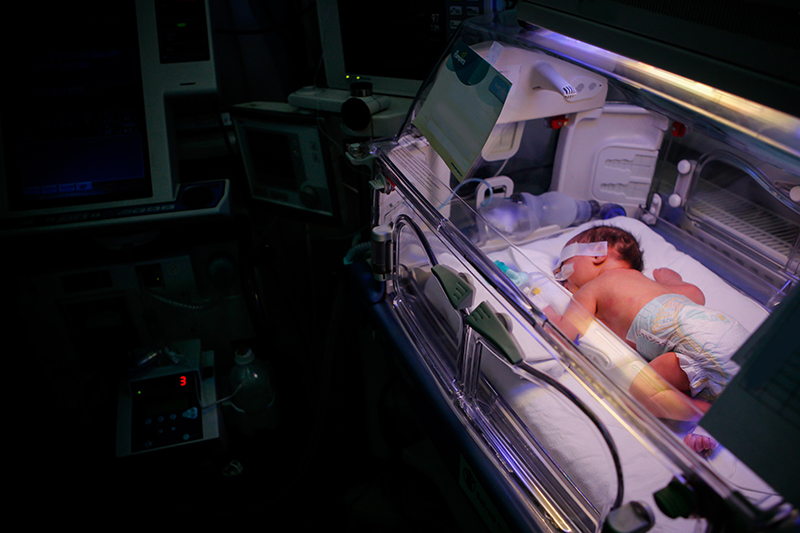
Each year, a team from Children’s of Alabama travels to Peru to provide cardiovascular surgeries through Heart Care International.
For Children’s of Alabama cardiac pediatric intensivist Santiago Borasino, M.D., traveling to Peru each year as part of a team providing cardiovascular surgeries to children offers him a special way to give back to his home country.
The trips are sponsored by Heart Care International, a nonprofit organization committed to saving the lives of children born with congenital heart defects. Volunteer medical teams come from cardiac centers throughout the United States, including Children’s of Alabama, to provide care throughout Latin America.
Borasino’s first trips were to Chiapas, Mexico, but since he learned about the organization’s work in Peru, he has focused his efforts there.

“I get to give back to my country,” he said. “There’s always a lot of guilt for leaving. And so I get to go there, help with surgeries and give back to the country some—a little bit. This teeny tiny bit probably doesn’t repay everything that the country has done for me, but it’s a little bit. It’s very special to me.”
The team—which most recently included Children’s cardiothoracic surgeon Robert Sorabella, M.D.; pediatric cardiac anesthesiologists Jack Crawford, M.D., Ph.D., and Patrick Hussey, M.D.; and Stephanie McBride, RNFA—works with doctors at the Instituto Nacional de Salud del Niño (INSN) San Borja in Lima, where Borasino was raised and attended medical school.
The local doctors coordinate with the visiting clinicians to choose the cases. “We can’t do cases that are too complex because we don’t have ECMO,” Borasino said. ECMO, or extracorporeal membrane oxygenation, is a life-support machine that can temporarily replace the heart and lungs. They also want the child to be able to recover before the team leaves, so they have to choose wisely, he added.
The visiting team works closely with their Peruvian counterparts. The American and Peruvian surgeons, anesthesiologists and nurses team up for surgeries, while Borasino partners with his Peruvian counterpart to manage the post-operative care side in the ICU. They generally perform about 15 surgeries a day.
Over his six trips to Peru, Borasino has witnessed significant growth in the skills and knowledge of the local medical professionals, most of whom were just starting to practice when he met them. “They’ve grown just like any doctor in the United States grows from being a young doctor who hasn’t done this too much to somebody who’s done it quite a lot.”
“The ultimate goal is that they will be independent,” he said. “They’re never going to be like Americans because of the resources. But, in theory, they could get close, at least for the moderate or low cases, a little complex but not too complex.”
Without these volunteer trips, the outlook for many of the young heart patients is grim. “Some of them will be lucky enough to get surgery within the system,” Borasino said. “And some of them will die. Not immediately, but eventually. Like in a few years without surgery, you end up dying. All these congenital heart diseases eventually kill you, either in weeks, months or years.”
However, the team’s work can be life-changing for the patients they’re able to help.
“The families are so thankful,” Borasino added. “Some come back every year when they know we’re there just to say hi, to bring their kids and tell us, ‘You saved our kid’s life.'” “It’s an opportunity to see more than just cardiac medicine,” he added. “And just to help.”