HC3 is led by Dr. Ahmed Asfari (top row, fourth from left) and Ashley Moellinger (top row, third from left).
Since the inception of the Heart Center Code Committee (HC3) in 2014, Children’s of Alabama’s cardiac arrest rate in the Cardiovascular ICU has fallen nearly 50%. The impact this committee has had on cardiac arrest reduction has come from numerous quality improvement initiatives and safety changes. In 2022, some of the initiatives Children’s implemented include the development of four guidelines, three communication enhancement tools, checklists and numerous safety changes.
Whenever a patient goes into cardiac arrest or a near miss is encountered, HC3 discusses the case. This multidisciplinary committee is composed of physicians, nurse practitioners, bedside nurses, respiratory therapists, cardiovascular operating room staff, chaplains and leadership from the heart center. HC3 meets every other week to evaluate each case, identify what was done well and areas for improvement.
Nurse practitioner Ashley Moellinger, CRNP, MSHQS, and cardiac intensivist Ahmed Asfari, M.D., who participate in quality improvement initiatives within the heart center, began leading the committee in 2021. They’ve focused on three key areas: education, inclusivity and innovation.
“We have unique patients with really complicated conditions that can be challenging to understand,” Moellinger said. “Whenever we review the event, we look for areas where there’s a knowledge gap or a need to enhance skills.” Then the team sends education briefs to the nurses to highlight committee findings.
Every nurse in the department is involved with the committee. “Really, the committee is owned by the nurses,” Moellinger said. An elite team of nurses reviews each case, interviews those involved and develops a presentation to tell the story of the event. Then, the committee decides together what they need to change. “And that’s where the education rollout comes into play,” Moellinger said.
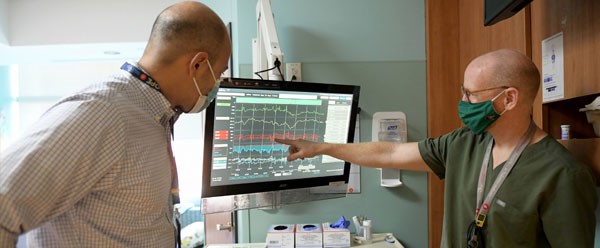
The committee uses artificial intelligence and near-real-time analytic algorithms to analyze cardiac arrest and near-arrest events. “When you’re talking about a cardiac arrest, everyone’s recollection is going to be different,” Asfari said. With the platform, “we can use objective data to show the patient’s course.” It also allows the team to view vital signs in a continuous manner on one screen.
“One of the things we are most proud of is the ‘green’ epinephrine action plan,” Asfari said. When a patient goes into cardiac arrest, epinephrine is one of the first medications administered, but it takes time to prepare the drug. Shorter time to administer it is associated with better outcomes. The action plan calls for prepared epinephrine at the bedside and includes standing orders for the nurse to administer it once the patient’s vitals reach a certain threshold. “It’s made a huge impact on our patient care,” he said. “Cardiac arrest is a real problem for children with cardiac disease because they are so fragile,” Asfari said. “Improving resuscitation and, more importantly, preventing the arrest can improve the outcome.”