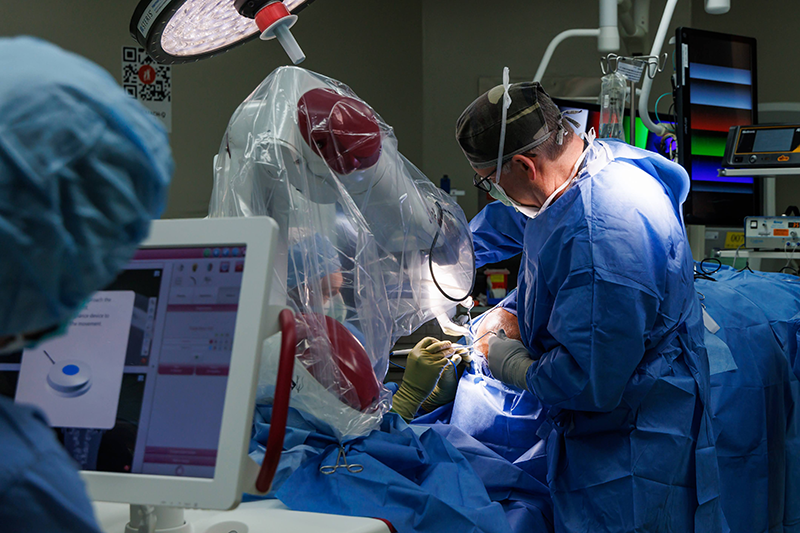
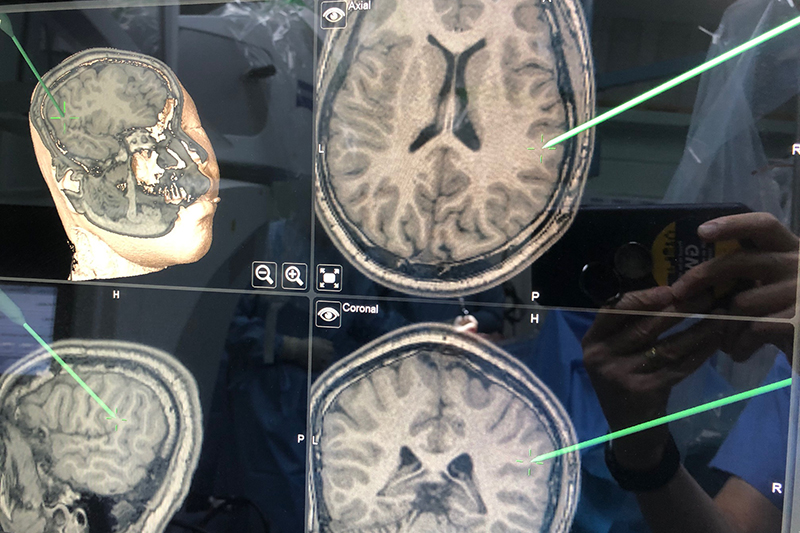
A new magnetoencephalography could improve treatment of multiple brain diseases at UAB and Children’s. (Photo by Andrea Mabry)
By Katherine Gaither, UAB
The complexity of the human brain has long been an enigma that neuroscientists have sought to untangle. Now, new technology at UAB will act as a critical tool to help researchers and clinicians interpret the brain in unprecedented ways.
UAB has recently invested in a new MEG, which stands for magnetoencephalography. It is used on pediatric and adult patients, so it benefits patients at both UAB and Children’s of Alabama. Put simply, MEG technology measures the magnetic fields that come from the brain’s nerve cells in an effort to analyze their function—and does so at millisecond intervals.
These implications are significant not only for localizing abnormalities in the brain in patients with diseases like epilepsy but also for studying how the brain performs normal functions like speaking, hearing, and seeing.
“It’s not invasive,” said Ismail Mohamed, M.D., professor in the UAB Division of Pediatric Neurology, Department of Pediatrics. “You don’t have to put electrodes in the brain, and it has no risks. You can potentially measure brain activity across multiple sessions. You can potentially measure them across a lifetime span. You can use it to learn things about how our brain functions.”
Measuring the brain’s magnetic fields
UAB was among the first medical centers in the country to obtain a MEG, having done so originally in 2001; however, evolving technology has created a need for replacing the old technology with a new one. The new machine was installed in September 2024.
Many are familiar with MRI as a form of imaging to interpret brain activity; however, having a MEG is not as common. UAB is one of fewer than 30 clinical centers in the nation that houses this technology.
“MRI looks at structure, but MEG primarily looks at the brain waves itself,” Mohamed explained.
The machine operates in a sealed room with a thick door, which eliminates outside magnetic noise. Patients lie or sit still during the scan, which takes precise magnetic field measurements of brain activity.
“The experience is not much different from laying inside an MRI scanner; however, the technology is quite different, and the way we measure is quite different,” Mohamed said. “It’s a passive measurement, which means that even if you’re pregnant, for example, you still can get a MEG scan. There are no risks.”
Compared to MRI and other brain scans like PET, and SPECT, the MEG gives you unique information about the brain as it tracks the activity of the nerve cells. EEG scans are similar, but the MEG has a heightened ability to localize this activity.
“A traditional EEG uses 25 electrodes. The MEG has 306 sensors,” Mohamed said. “So that coverage of the brain is bigger, it enhances the potential to produce more accurate information.”
According to Benjamin Cox, M.D., assistant professor in the UAB Department of Neurology, the difference is also electric vs. magnetic.
“The electrical fields that EEGs are recording are very much attenuated by the skull and all the intervening tissues,” Cox said. “The magnetic fields are not. So, we get a lot more precise localization with the MEG.”
Clinical implications
One significant implementation of the MEG is for use in epilepsy surgery to determine where in the brain seizures originate. Surgeons can use the results of a MEG scan to plan epilepsy surgeries.
“When we’re doing epilepsy surgery and trying to figure out if patients are a surgery candidate, we need to know exactly where the seizures are coming from as precisely as possible, and many times we end up putting electrodes in the brain to sample that activity directly,” Cox said. “So having studies like MEG, where we can have a precise idea of where to put those electrodes, is very helpful.”
Kristen Riley, M.D., professor in the UAB Department of Neurosurgery, notes that “MEG studies help us as surgeons to localize seizure onset zones, directing us to areas to implant monitoring electrodes. Often these areas look completely normal on MRI, but are identified by the MEG study as possible sites of seizure onset.”
A second clinical implementation involves functional brain mapping—to localize areas important for language, sensory and motor function.
“It has huge implications for learning, like child development,” Mohamed said. “Learning new languages. Processing information as the child grows. It also has a lot of potential research use for the prediction of disease outcomes. Studying things like dementia or Alzheimer’s disease.”
Cox added that the new MEG’s presence within UAB Hospital creates advantages for patients and clinicians when used as an inpatient procedure instead of an outpatient procedure, as it has been in the past.
“Epilepsy patients are on seizure medicines on a day-to-day basis to prevent seizures from happening,” Cox said. “When we bring them into the hospital and evaluate them for surgery, we get them off of their medicines, which increases epileptic activity in the brain, so it will hopefully increase the likelihood we record epileptic activity during the MEG scan.”
Studying epilepsy less invasively
From a research perspective, Rachel Smith, Ph.D., assistant professor in the UAB Department of Electrical and Computer Engineering, had been using the existing MEG to validate methods that she has been developing for intracranial EEG in epilepsy patients through a project funded by CURE Epilepsy.
“We’re electrically stimulating a given brain region and then looking for responses in the rest of the brain,” Smith explained. “That is helping us build these unique brain networks. So, we know if we stimulated in one region and see a response in another region, that means that those two regions are likely functionally or anatomically connected in some way.”
Smith and her team are then using MEG data to build computer models that can hopefully test neurophysiological signals virtually to localize epileptic seizures—and therefore less invasively.
“We’re actually saying, let’s build a network from MEG data and see if we can do a virtual stimulation where we actually just stimulate in the computer model and not in real life and see if we can get the same clinical information out,” Smith added.
The new MEG will be a useful tool for advancing research into the future; however, researchers are already realizing significant research implications with the new technology.
“It’s going to be really helpful and translational for a lot of patients right now,” Smith said. “I think being one of 27 centers across the U.S. that has access to this in our hospital is a huge opportunity for people here at UAB to take advantage of. We’re really excited.”