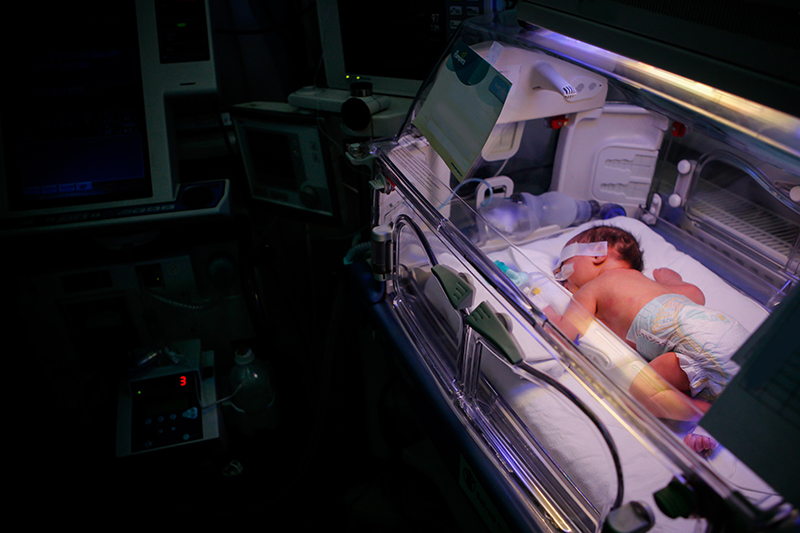
Studies led by Children’s neonatologists show early indicators of bronchopulmonary dysplasia with pulmonary hypertension.
It’s well-known that preterm infants are prone to breathing difficulties due to their underdeveloped lungs. But the most common lung disease in these babies, bronchopulmonary dysplasia (BPD), is only recently becoming better understood more than a half-century after it was first described.
Now, Children’s of Alabama neonatologist Samuel Gentle, M.D. is expanding that knowledge by focusing on the most severe type of BPD—the form associated with pulmonary hypertension (PH)—in research that teases out contributing factors to this deadly disease.
It’s a major threat: nearly half of preterm infants develop BPD, which can lead to long-term breathing and health problems. About 20% of these babies also develop PH, and an estimated 40% of them will die of BPD-PH before turning 2 years old.

“This is a disease for which there’s growing research interest. It can be lethal, is not uncommon in extremely preterm infants, and we have little understanding of how to prevent or treat it,” said Gentle, who’s also an assistant professor of neonatology at the University of Alabama at Birmingham (UAB). “And children who do survive have long-term complications that persist into adulthood. It’s not a disease they just grow out of.”
“I’ve also had many interactions with families who lost a child to this,” he added. “Oftentimes, a child will be stable and doing well, and then collapse. I’ve seen how this can ravage a family.”
Since research has been scant about what causes the development of BPD-PH—as well as how to screen, treat and prevent it—Gentle wanted to fill the vacuum. Currently, a single ultrasound of the heart is the standard diagnostic method, though UAB performs this testing more frequently.
“We need to get better at identifying this disease in real time, rather than doing ultrasounds at arbitrary time intervals,” Gentle said. “Even with UAB’s testing approach, I believe it will become possible to diagnose it sooner, allowing earlier initiation of PH-targeted therapies.”
Along with UAB colleagues, Gentle published two studies that assessed factors that may contribute to BPD-PH in preterm babies. Published in the American Journal of Respiratory and Critical Care Medicine, they found two important associations: The duration of intermittent hypoxia events and the presence and persistence of a patent ductus arteriosus (PDA) after birth are both novel risk factors for BPD-PH.
In the first study, Gentle found that infants who experienced intermittent hypoxia events lasting longer than one minute were twice as likely to develop BPD-PH. “If an infant has longer intermittent hypoxia events, we might be more proactive in screening that infant for BPD-PH,” he said.
In the second study, preterm babies born with BPD-PH between 22 and 28 weeks’ gestation were more likely to have a PDA vessel that stayed open longer than 28 days. Babies with longer PDA duration were also more likely to die due to complications of BPD-PH than infants with only BPD. “The PDA could be interfering with the development of pulmonary vasculature resulting in PH,” Gentle said.
UAB will be participating a multicenter trial to determine whether closing PDAs with a catheter-closure device might lower the risk of this PH variant. But far more study is needed, Gentle pointed out.
“While this research focused on a specific phenotype of BPD, we need a comprehensive approach to identifying each infant’s specific type of lung disease from which we can decide on the best therapeutic course for every child,” he said.

No Comments